Breast cancer is characterized by the abnormal transformation and uncontrolled growth of cells within the breast tissue. Initially localized, these changes can eventually become harmful to the body. It is the most common type of cancer among women, particularly prevalent in Western societies. Statistics indicate that 1 in 8 women in these regions will develop breast cancer at some point in their lives.
Early diagnosis plays a critical role in managing breast cancer. Detecting the disease in its early stages allows for less invasive treatments and significantly reduces its impact on the patient. Therefore, identifying high-risk groups and emphasizing early detection is crucial to preventing harm.
While breast cancer predominantly affects women, it can also occur in men, albeit at a much lower frequency.
What Causes Breast Cancer?
The exact cause of breast cancer remains unknown. Approximately 80-90% of cases have no identifiable cause, while about 10% are linked to familial and genetic factors. Individuals with specific genetic mutations, such as BRCA1 and BRCA2, have a significantly higher risk—up to 70%—of developing breast cancer, especially after the age of 40. For this reason, families with a history of early-onset breast cancer, bilateral breast cancer, or male breast cancer should undergo thorough evaluation.
Genetic testing is recommended for individuals diagnosed with breast cancer. If a genetic mutation is identified, it is advised that other family members undergo testing as well. If these mutations are detected in relatives, preventive measures can be taken. These may include close monitoring, protective medications, or, in some cases, preventive surgeries such as removing breast tissue, which has been popularized by Angelina Jolie’s case.
In addition to genetic factors, advanced age, obesity (especially after menopause), stress, and environmental factors are also associated with an increased risk of breast cancer.
Interestingly, women who maintain a healthy weight and engage in regular exercise are observed to have a lower risk of developing breast cancer.
How Common Is Breast Cancer?
The frequency of breast cancer varies depending on the region. For instance, in Western countries such as the United States and Europe, 1 in 8 women is diagnosed with breast cancer. In contrast, it is much less common in Japan, likely due to differences in diet, environmental factors, and body weight. Genetic predisposition also plays a significant role in the risk of developing breast cancer.
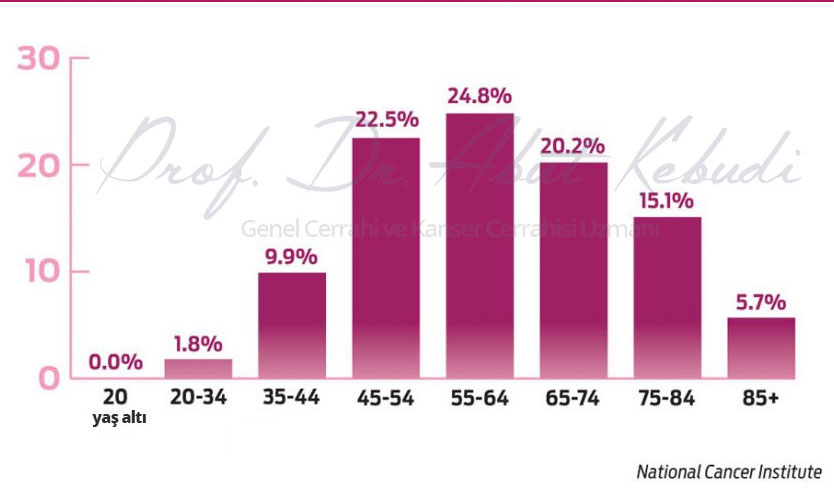 In Turkey, the frequency is lower than 1 in 8 women. However, there are regional differences: in the eastern parts of the country, breast cancer is less common but tends to be diagnosed at more advanced stages. In contrast, in the western regions, cases are detected earlier, which improves outcomes.
In Turkey, the frequency is lower than 1 in 8 women. However, there are regional differences: in the eastern parts of the country, breast cancer is less common but tends to be diagnosed at more advanced stages. In contrast, in the western regions, cases are detected earlier, which improves outcomes.
Interestingly, Japanese individuals who have migrated to the United States show higher rates of breast cancer, potentially due to changes in diet, stress levels, and environmental influences. Additionally, Ashkenazi Jews are another group with notably high breast cancer rates.
These observations suggest that breast cancer prevalence is influenced by a combination of factors, including ethnicity, genetics, environmental conditions, and dietary habits.
How Is Breast Cancer Diagnosed Early?
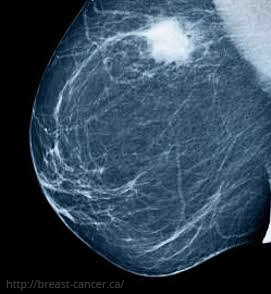 Early detection of breast cancer has a significant positive impact on a patient’s future health. According to the World Health Organization’s recommendations, women aged 20-40 should visit a breast specialist every three years, even if they have no symptoms. After the age of 40, these check-ups should occur annually. Additionally, women are encouraged to perform regular monthly self-examinations.
Early detection of breast cancer has a significant positive impact on a patient’s future health. According to the World Health Organization’s recommendations, women aged 20-40 should visit a breast specialist every three years, even if they have no symptoms. After the age of 40, these check-ups should occur annually. Additionally, women are encouraged to perform regular monthly self-examinations.
From age 40 onwards, screening mammograms are crucial. While opinions vary on the frequency, most guidelines recommend mammography either annually or every two years. Regular screening can detect breast cancer at an early stage, or even identify precancerous changes before the disease fully develops, increasing the chances of successful treatment.
The Importance of Early Detection in Breast Cancer
Early detection in breast cancer is critical. When diagnosed early, the disease can often be treated with less intensive methods, reducing its impact on the patient’s life and preventing severe long-term consequences.
With early detection, treatment is typically less invasive and can lead to full recovery, as the cancer has not spread. Additionally, surgery performed at an early stage is usually more minimal, preserving the breast’s structure and achieving better cosmetic outcomes. In summary, early detection ensures lighter treatment, better aesthetic results, and a brighter future for the patient.
Which Doctor Should You Consult for Suspected Breast Cancer?
If breast cancer is suspected, the ideal doctor to consult is a general surgeon specializing in breast diseases. These specialists handle all aspects of the diagnosis and treatment process, including examinations, ordering and interpreting imaging tests, performing biopsies if necessary, and coordinating care with an oncologist.
Since surgical intervention is typically the first step in treatment unless the cancer has progressed significantly, it is essential to consult a general surgeon experienced in breast diseases for timely and effective care.
Methods of Diagnosing Breast Cancer
Breast cancer can be diagnosed through various methods, often initiated by the patient noticing symptoms such as a lump in the breast, redness on the breast skin, nipple discharge, or swelling in the armpit. Alternatively, a doctor may detect these signs during a routine examination, even in the absence of symptoms.
Doctors also rely on imaging techniques such as mammography, ultrasound, and, if needed, MRI to evaluate the breast and armpit areas. These tools are particularly useful for detecting abnormalities that may not be palpable.
The final step in diagnosis is a biopsy, which involves collecting a tissue sample for analysis. Whenever possible, fine-needle aspiration or core needle biopsy is preferred over surgical biopsy. While surgical biopsy may be necessary in some cases, needle-based methods are less invasive and are generally recommended.
In summary, breast cancer diagnosis involves:
- Self-examination by the patient.
- Physical examination by the doctor.
- Radiological imaging of the breast.
- Biopsy for definitive confirmation.
Who Is at Risk for Breast Cancer?
Being a woman is the primary risk factor for breast cancer, as it is 100 times more common in women than in men. Other significant risk factors include advanced age and being postmenopausal. However, the most critical risk factor is having a first-degree relative (mother, sister, or daughter) with breast cancer. Although not everyone with a family history of breast cancer will develop the disease, familial cases account for approximately 10-15% of all breast cancers, with some linked to genetic mutations.
Genetic factors, such as mutations in the BRCA1 and BRCA2 genes, are well-known contributors. Testing for these mutations in individuals diagnosed with breast cancer is crucial, as it helps assess the risk for siblings and future generations.
The risk is especially elevated in individuals with:
- A first-degree relative diagnosed at a young age.
- Bilateral breast cancer (cancer in both breasts).
- Male breast cancer in the family.
Understanding these risk factors allows for better monitoring and early intervention strategies.
For individuals with a family history of breast cancer, undergoing genetic testing is crucial. If a genetic mutation or abnormality is identified, other family members who have not developed breast cancer should also be tested.
These tests can help prevent the onset of the disease or ensure that any cancer is detected at an early stage, minimizing its impact. By identifying genetic risks in advance, it is possible to protect family members from the adverse effects of breast cancer and provide timely preventive measures.
Approach to Non-Palpable Breast Masses
Non-palpable breast masses require a distinct approach within breast health management. When a patient or doctor detects a lump during physical examination, diagnosis and treatment are relatively straightforward. However, in cases where the patient has no symptoms and no findings are evident upon examination, but imaging techniques like mammography or ultrasound reveal a suspicious area, a different strategy is needed.
Because these masses cannot be felt and their exact location is harder to determine, diagnostic and treatment procedures must be more precise. In the past, when medical techniques were less advanced, suspicious areas in the breast were removed based on estimates, which sometimes led to incomplete excision or missed cancerous tissue, as revealed in subsequent imaging.
Today, advanced methods such as image-guided localization enable accurate marking of the suspicious region, ensuring precise identification and removal of the affected tissue. This progress significantly improves both diagnostic accuracy and treatment outcomes for non-palpable breast lesions.
Marking Non-Palpable Breast Masses
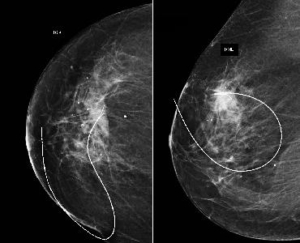 Non-palpable breast lesions hold significant importance, as they often represent the earliest stages of cancer. Identifying and closely evaluating such lesions enables early detection of cancer or precancerous changes, offering the opportunity to treat the condition at its earliest stage.
Non-palpable breast lesions hold significant importance, as they often represent the earliest stages of cancer. Identifying and closely evaluating such lesions enables early detection of cancer or precancerous changes, offering the opportunity to treat the condition at its earliest stage.
This approach significantly increases the chances of the patient maintaining a normal, healthy life.
Approach to Breast Lesions
When addressing breast lesions, the process typically begins with the patient noticing symptoms such as a lump, nipple discharge, redness on the breast skin, or swelling in the armpit. In other cases, a doctor may detect these findings during routine check-ups, even if the patient has no complaints. Additionally, imaging studies, especially after age 40, may reveal abnormalities such as structural changes or calcifications in the breast tissue, warranting further investigation.
If a suspicious area is identified, a biopsy is performed to determine whether the lesion is benign or malignant. Modern techniques often prefer fine-needle aspiration or core needle biopsy for this purpose, as initial open surgery for diagnosis may complicate subsequent treatments.
In cases where the exact location of a small lesion is unclear, advanced localization techniques, such as wire-guided marking, are employed. This ensures that only the affected area is precisely removed during surgery, minimizing unnecessary tissue removal.
Key Methods for Identifying Breast Abnormalities:
- Clinical Examination – Identifying abnormalities during self-checks or professional exams.
- Imaging – Using mammograms, ultrasounds, or MRIs to detect structural changes.
- Biopsy – Confirming the nature of the lesion with needle or core sampling.
Accurate diagnosis and treatment of breast lesions rely on a combination of these methods, ensuring effective and targeted care.
Imaging Methods for Breast Cancer Diagnosis
Mammography is considered the gold standard for evaluating breast conditions. It is not recommended before the age of 30–35 due to the sensitivity of younger breast tissue. Starting at age 40, annual or biennial mammograms are advised for early detection of breast cancer.
- Ultrasonography: For younger women, ultrasound is often the first imaging choice. It is effective in evaluating breast tissue and can provide diagnostic clarity, especially in dense breasts.
- MRI (Magnetic Resonance Imaging): Breast MRI is useful for detecting cancerous areas, particularly in high-risk patients or younger individuals. It provides detailed imaging and can complement other methods when necessary.
- Combined Approaches: Combining mammography with ultrasound enhances diagnostic accuracy, offering better results by compensating for the limitations of each individual method.
By utilizing these imaging techniques appropriately, breast cancer can be detected early, increasing the likelihood of effective treatment and improved outcomes.
What is Fine-Needle Aspiration Biopsy (FNAB) in Breast Cancer Diagnosis?
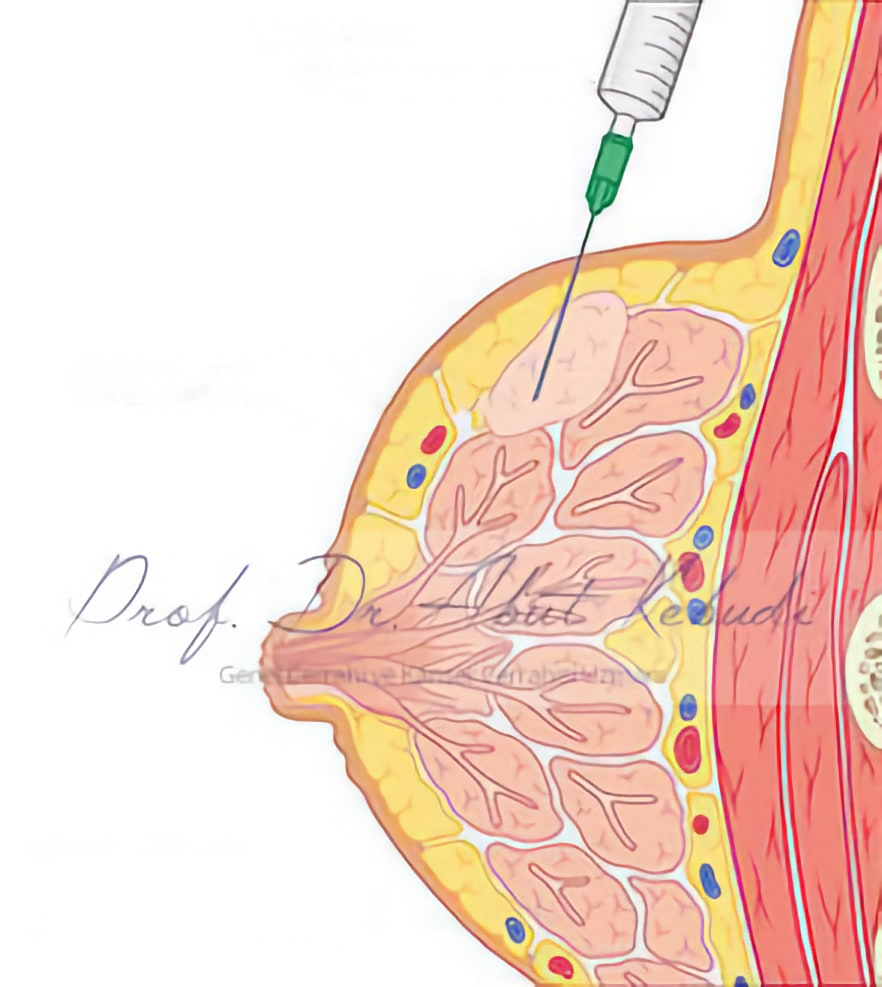 Fine-needle aspiration biopsy (FNAB) involves obtaining cells from the breast tissue for diagnostic purposes. Here’s how it works:
Fine-needle aspiration biopsy (FNAB) involves obtaining cells from the breast tissue for diagnostic purposes. Here’s how it works:
- A thin needle is inserted into the breast tissue.
- Negative pressure is applied using a syringe to extract a small number of cells.
- The cells are transferred onto a glass slide, stained with special dyes, and examined under a microscope.
- If tumor-specific structures are identified, a definitive diagnosis can be made.
This minimally invasive method provides quick diagnostic results and plays a vital role in determining the nature of a suspicious breast lesion.
What is Core Needle Biopsy in Breast Cancer Diagnosis, and How is it Performed?
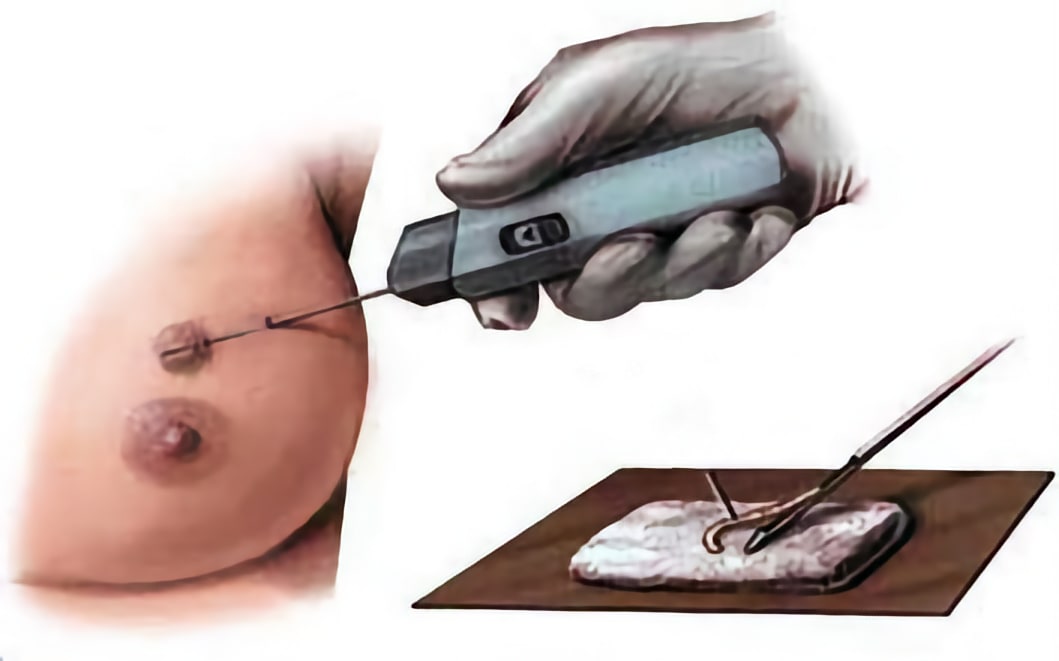 Core needle biopsy is a more advanced and effective diagnostic method compared to fine-needle aspiration biopsy. In this technique, a special device is used to obtain a tissue sample from the breast.
Core needle biopsy is a more advanced and effective diagnostic method compared to fine-needle aspiration biopsy. In this technique, a special device is used to obtain a tissue sample from the breast.
How It Works:
- The biopsy device is pressed against the breast at the site of the suspicious lesion.
- With the press of a button, the device extracts a small cylindrical tissue sample.
- Unlike fine-needle aspiration, which collects only cells, core needle biopsy retrieves tissue samples.
Why Is Core Needle Biopsy Important?
- Tissue samples provide detailed information, making it easier to establish a diagnosis.
- Specific tumor characteristics, such as type and grade, can also be determined from the collected tissue.
Core needle biopsy is considered the gold standard for accurate breast cancer diagnosis today. Its ability to provide comprehensive information about the tumor makes it indispensable in modern breast cancer diagnostics.
How is Breast Cancer Staged?
Breast cancer staging is determined using the international TNM system, which assesses three key factors:
- T (Tumor): Indicates the size and extent of the primary tumor.
- N (Nodes): Refers to the involvement of lymph nodes.
- M (Metastasis): Identifies whether the cancer has spread to distant organs.
Based on these criteria, breast cancer is categorized into four main stages:
- Stage 1: Early-stage cancer; the tumor is small, and there may be no lymph node involvement or distant spread.
- Stage 2: The tumor may be larger and/or involve nearby lymph nodes but has not spread to distant sites.
- Stage 3: Advanced local cancer with significant lymph node involvement or larger tumors.
- Stage 4: Cancer has metastasized to distant organs, such as the lungs, liver, or bones.
Why is Staging Important?
Early-stage cancer (Stage 1 or 2) is typically easier to treat and offers better outcomes. Accurate staging guides the treatment plan, including surgery, chemotherapy, radiation, or targeted therapies, and helps predict prognosis.
In summary, the earlier the stage, the more straightforward the treatment and the better the long-term results.
Approach to Early-Stage Breast Cancer
In early-stage breast cancer, less invasive treatments yield excellent outcomes, allowing patients to return to a nearly normal life. Moreover, cosmetic results are significantly improved with limited surgical approaches, preserving the breast’s appearance.
Advances in Surgical Techniques
- Previously, complete breast removal (mastectomy) was standard for all breast cancer cases.
- Today, with updated surgical concepts and techniques, removing only the tumor and surrounding tissue (breast-conserving surgery) is often sufficient for early-stage cancers.
- This approach preserves the breast’s natural appearance while ensuring effective treatment.
Axillary Lymph Node Management
- The armpit area (axilla) plays a critical role in breast cancer surgery.
- During surgery, sentinel lymph node biopsy or specialized tests are used to check for cancer spread.
- If no cancer is detected, removing all axillary lymph nodes (a procedure with significant side effects) can be avoided.
Benefits of Early Detection and Treatment
- Patients receive less aggressive treatments with fewer complications.
- The breast’s natural appearance is maintained, contributing to better psychological and cosmetic outcomes.
- A more normal lifestyle is achievable, with excellent long-term prognosis.